Ostomy
An ostomy is a surgically created opening in the abdomen that allows waste to exit the body through a stoma when the natural route is no longer possible or safe. It saves lives, protects healing tissues, and can dramatically improve quality of life.
Temporary ostomies protect the bowel after surgery or inflammation.
Permanent ostomies replace damaged or cancerous sections of bowel or bladder.
Common reasons someone needs an ostomy include:
- Colorectal cancer (most common)
- Advanced Crohn’s disease or ulcerative colitis
- Trauma or perforation of bowel
- Diverticulitis complications
- Bowel obstruction or severe infection
- Bladder cancer (urostomy)
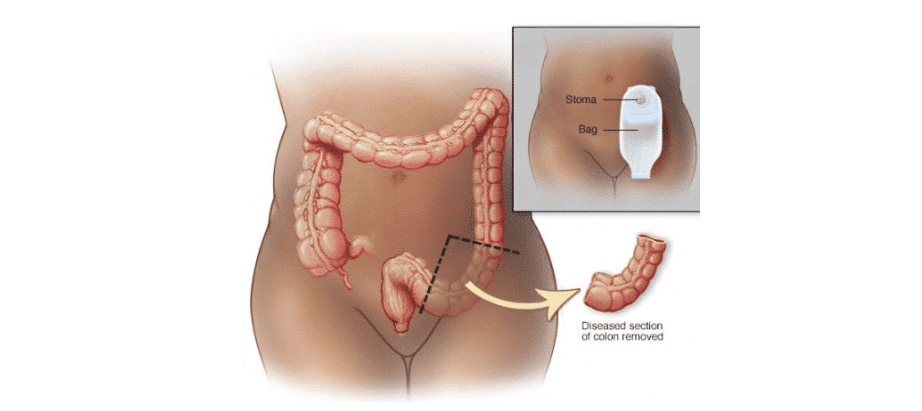
Sources: Cleveland Clinic • Mayo Clinic • UOAA
Types of Ostomies
| Type | Location | Output | Used For | Key Differences |
|---|---|---|---|---|
| Colostomy | Large intestine (colon) | Formed or semi-formed stool | Cancer, diverticulitis, trauma | May irrigate for predictable bowel pattern |
| Ileostomy | Small intestine (ileum) | Liquid to paste-like output | Crohn’s, UC, genetic polyposis | Higher risk of dehydration & blockage |
| Urostomy | Urinary diversion | Continuous urine flow | Bladder cancer, neurogenic bladder | Requires night drainage bag |
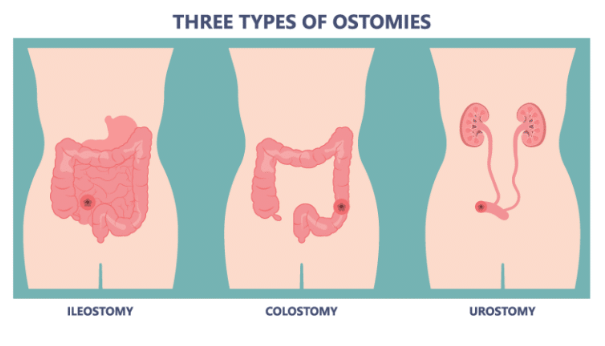
Ostomy Meaning & Medical Definition
An ostomy (medical term: ostomy surgery) is a surgical procedure that creates an artificial opening, called a stoma, in the abdomen to divert waste (stool or urine) from the body when the normal pathway is damaged or removed.
According to the United Ostomy Associations of America (UOAA) and Mayo Clinic, an ostomy is life-saving for conditions like colorectal cancer, inflammatory bowel disease (Crohn's or ulcerative colitis), bladder issues, or trauma.

Ostomies (plural) can be temporary (to allow healing) or permanent. The opening is called a stoma, and waste collects in an external pouch (ostomy bag).
What is a Stoma? (Medical Term Explained)
A stoma is the actual opening created during ostomy surgery – a small, pink/red piece of intestine brought to the surface of the abdomen. It's painless (no nerve endings) and allows waste to exit the body.

The stoma is rosebud-shaped, moist, and about 1-2 inches wide. It may protrude slightly or lie flat.
- Stomas are created from healthy bowel tissue
- No sensation – you don't feel waste passing
- Requires a pouch (ostomy bag) to collect output
What is an Ostomy? Complete Guide
What is an ostomy? It's a surgical diversion that bypasses damaged parts of the digestive or urinary tract. The three main types are:
| Type | Description | Output | Common Reasons |
|---|---|---|---|
| Colostomy | Opening in large intestine (colon) | Formed stool | Colorectal cancer, diverticulitis |
| Ileostomy | Opening in small intestine (ileum) | Liquid/paste stool | Crohn's disease, ulcerative colitis |
| Urostomy | Urine diversion (ureters to stoma) | Continuous urine | Bladder cancer, birth defects |

With modern accessories like SIIL covers and belts (UOAA recommended), most people return to normal activities – work, sports, travel, intimacy.
Ostomy Surgery: What to Expect
Before Surgery
- Stoma site marking by a WOCN nurse
- Pre-op education: pouching, skin care, lifestyle changes
- Stopping certain medications
- Bowel prep if required
During Surgery
- Performed under general anesthesia
- May be open or laparoscopic
- Damaged bowel/organ removed, healthy section brought to surface
- Stoma shaped and matured
After Surgery
Patients usually stay in the hospital for 3–7 days. Full recovery takes 6–8 weeks.

Daily Life With an Ostomy
Ostomy Pouch Systems
- One-piece: flange + pouch combined
- Two-piece: flange separate; easier on sensitive skin
- Change every 3–7 days
- Empty when 1/3 to 1/2 full
Food & Diet for ostomates
:max_bytes(150000):strip_icc():format(webp)/VWH-EllenLindner-PostColostomyColectomyDiet-4000x2700-eb2602aed1da4db7943be2d1e7375f6f.png)
Source: Mayo Clinic
Sports, Work & Physical Activity with a stoma bag
Most activities are safe once fully recovered.
- Walking, yoga, swimming, cycling
- Contact sports: use a stoma protector
- Weightlifting: start slow; wear a hernia belt

Travel with an Ostomy
- High-waisted clothing helps support and conceal the pouch
- Pack at least double your normal supplies when flying
- TSA allows ostomy supplies; doctor’s note optional

Intimacy & Confidence with an ostomy
Intimacy is absolutely possible and healthy after an ostomy. Emotional readiness matters more than the timeline.
- Empty the pouch beforehand
- Use ostomy wraps, pouch covers or lingerie
- Try side-lying positions for comfort

Possible Complications
Seek medical help immediately if you experience:
- No stoma output for 6+ hours
- Severe or worsening pain
- Redness, swelling or pus around stoma
- High fever
- Unusual or foul odor
Ostomy Reversal & Long-Term Outlook
Many temporary ostomies are reversible depending on the amount of healthy bowel remaining.
Long-term, most people live full, active lives — traveling, working, exercising, and enjoying relationships fully.
Deep Learning: Live Better With Your Ostomy
This section expands your knowledge with medically verified insights, emotional support, and practical strategies for long-term wellness with an ostomy.
1. The First 30 Days After Ostomy Surgery
The first month is about healing, learning new routines, and building confidence. Most people feel overwhelmed at first — this is normal and temporary.
- Expect normal swelling and changes in stoma size
- Practice pouch changes with a nurse before going home
- Use mirror positioning to build confidence
2. Skin Care & Protecting the Peristomal Area
Healthy skin should look like the rest of your abdominal skin — not red, itchy, or weepy.
- Ensure the flange opening fits 1–2 mm around the stoma
- Use barrier rings for irregular stoma shapes
- Address leaks immediately to prevent irritation
3. Preventing Ostomy Hernias
Hernias occur when weakened abdominal muscles bulge near the stoma. Prevention is key.
- Avoid heavy lifting for 8–12 weeks
- Use an ostomy support belt during movement
- Strengthen the core with gentle exercises
4. Managing Gas, Odor & Bloating
- Chew slowly and avoid drinking through straws
- Limit high-gas foods (broccoli, beans, carbonated drinks)
- Use deodorizing drops for odor control
5. Sleeping Better With an Ostomy
- Side sleeping is often most comfortable
- Use a small pillow for support near the stoma
- Empty the pouch before bedtime
6. Body Image, Confidence & Mental Health
Emotional healing is as important as physical healing. Talking openly with partners and connecting with other ostomates can dramatically improve confidence.